Maternal Health Awareness Day 2024
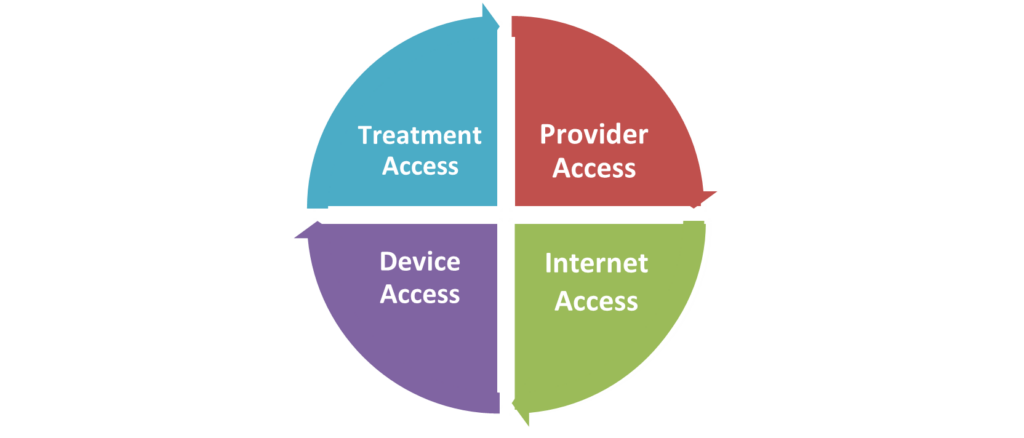
Today is, National Maternal Health Awareness Day 2024. This year the focus is on Access to Care. Access in Crisis.
Posted under: Maternal Health, Quality of Care
This year the focus is on Access to Care. Access in Crisis.
And that is true. For many rural communities, closures of obstetric units and hospitals have created tremendous burdens in obstetric availability. Medicaid reimbursement has created significant voids in hospital budgets that are no longer sustainable. Insurance costs have created chasms in care, leading to a lack of obstetric specialists and delivery options in states least likely to afford lapses in care.
But there is more to accessing high-quality maternal care than we realize. Or recognize. Or care to admit. I will give you a few examples that create challenges to accessing even the most well-supported maternal care sites.
1. Racial disparities and racism: In April 2023, the Centers for Disease Control published Maternity Care Experiences that revealed troubling facts (survey methodology available within the CDC document):
- 30% of Black, Hispanic, and multiracial mothers reported mistreatment (e.g., violations of physical privacy or verbal abuse) during maternity care.
- 40% of Black, Hispanic, and multiracial mothers reported discrimination during maternity care.
- 45% of all mothers reported holding back from asking questions or discussing concerns with their provider.
Researchers from the University of California at San Francisco found that “racialized pregnancy stigma may result in reduced access to quality health care; barriers to services, resources, and social support; and poorer psychological health”.
The experiences of Black women at the intersection of race, gender, and pregnancy | Bixby Center for Global Reproductive Health (ucsf.edu)
2. Obesity stigma: The stigma associated with obesity continues to impact a woman’s or birthing person’s choice of providers, or their willingness to seek out care. Obesity stigma is fueled by misconceptions and assumptions about people with obesity and continues to exist today. Have you ever seen a colleague or co-worker roll their eyes upon receiving the report of a pregnant patient with severe obesity? Have your own eyes rolled? What assumptions do you make about weight? And how are these assumptions keeping women and birthing people from accessing care due to obesity stigma from healthcare providers?
3. Mental health stigma: The stigma that continues to permeate healthcare is that of mental health disorders. “The bipolar patient in room 3…” Have you heard that recently? Ever? In 2019, researchers in California reviewed 300 records of women who died within one year of giving birth. The second leading cause of death was substance use disorder. Two-thirds of these women had at least one (1) interaction with the healthcare system. Are we seeing despair? Are we making assumptions about maternal mental health? Check out the Maternal Mental Health Leadership Alliance for more information.
4. Homelessness: Back in 2022, I wrote a blog entitled Homelessness is Not Neglect. There is incredible stigma that is associated with homelessness, and more particularly pregnant women who are homeless. Between assumptions, misconceptions, and other issues that can taint perception, homelessness can be a significant deterrent to seeking maternal health care. Here is a quote from the blog I wrote, and it is just as important now as it was then:
“Members of our team immediately called CPS on a Black mother for being homeless. She left AMA during labor, and we do not know where she delivered. I was so distraught. Our policy directs us to contact CPS for homeless parents. Like they have not been traumatized enough already. We must change our policies to protect these mothers and families and make every effort to keep these newborns with their mothers.”
5. Incarceration: According to Knittel et al (2022), “We Don’t Wanna Birth It Here”: A Qualitative Study of Southern Jail Personnel Approaches to Pregnancy: Women & Criminal Justice: Vol 33, No 5, approximately 55,000 pregnant people are incarcerated in jails each year. As many of these people are of childbearing age, it would stand that some of these people would deliver while incarcerated. In 2018, Black women were incarcerated at twice the rate of white women (Equitable Care for Pregnant Incarcerated Women: Infant Contact After Birth - A Human Right (umich.edu)). This commentary by Franco et al provides a bleak picture of maternal health in our carceral systems. I would strongly encourage the review of this paper and learn more about how to advocate for maternal health patients who experience incarceration. Not only is there stigma of patients during their period of incarceration, but also upon release and their re-entry into their community.
Access to care can mean many things. But one thing is certain. Access to high-quality, affordable, and available care in the community can be life-sustaining and life-changing. Let’s improve maternal health everywhere. Every patient, every time, everywhere.
National Maternal Health Awareness Day 2024